 In an earlier post we talked about some of the research on appetite. We reviewed some of the peptide hormones that regulate appetite and how the entire system that controls appetite is really designed to cope better with a time of scarcity than a time of plenty.
In an earlier post we talked about some of the research on appetite. We reviewed some of the peptide hormones that regulate appetite and how the entire system that controls appetite is really designed to cope better with a time of scarcity than a time of plenty.
Here I want to talk more specifically about the interplay between other hormone systems and appetite and weight regulation.
This part of the overall set of articles on appetite and body composition focuses on hormone systems that are not specifically designed to control appetite, but do so because changing body composition or diet is important for other reasons. For example, having better availability of quick energy stores like glucose when facing challenges.
Broadly we will consider these hormone systems –
- The cortisol system – your stress hormones.
- The thyroid system – your body’s overall metabolism regulator.
- Sex hormones and their relationship to body composition.
- The insulin system which controls blood glucose.
The Cortisol System

Cortisol plays a large role in regulating many functions throughout the body. It is best known as the “stress” hormone, and, these days, with lives that have relatively few imminent dangers, discussion about cortisol mostly focuses on things that it does that are bad for us.
However, it plays a central role in the body’s ability to adapt to almost any stressful situations – illness, injury, external threats – and it is worth beginning this discussion by reflecting on the fact that we could literally not survive without an intact cortisol system.
As with many hormone systems, cortisol is regulated in a complicated way that starts with the brain (hypothalamus) and proceeds to a part of the body that is midway between brain and hormone gland (the anterior pituitary) and then ends up with the hormone glands themselves (the adrenal cortex).
In terms of its effects on appetite and body composition, think of cortisol as the system whose philosophy is – use it now because this struggle is a matter of life and death.
So, high cortisol levels draw down on all of the body’s long term stores of energy and shifts the overall body metabolism away from building and regenerating (things like muscles, skin, etcetera) and towards an immediate ability to use large amounts of energy to deal with a crisis.
The main sources of this kind of energy are glucose and fatty acids. So high cortisol levels tend to result in higher blood glucose and fatty acid levels (cholesterol, triglycerides).
Other effects are –
- Cortisol stimulates the release of insulin and has a role in maintaining blood sugar levels
- It makes you want to eat a lot
- It causes cravings for sweets and simple carbohydrate foods that cause insulin levels to spike and then plummet quickly, which makes you hungrier
- Tends to cause increased deposition of “stress fat”, which is concentrated in the abdominal stomach area
The Thyroid System
The thyroid system is all about overall body metabolism. Think of it as the dimmer switch for the body’s energy 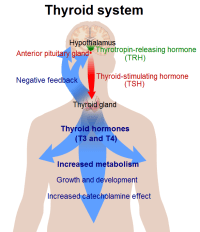 systems.
systems.
High levels of thyroid stimulate increased activity and energy. Low levels of thyroid turn off energy and activity systems.
Based on that, you might not be surprised to learn that one of the main symptoms of high or low thyroid is sweating and feeling hot (hyperthyroidism) and abnormally low sweating and feeling cold (hypothyroidism).
Just as with the cortisol system. There are three steps involved in regulating thyroid hormone release: they hypothalamus, the anterior pituitary and the thyroid gland itself.
This may help to explain one of the most common misunderstandings about thyroid test results.
“Doc, why do you say my thyroid is low if my TSH (thyroid stimulating hormone) is too high?”
If the thyroid gland starts to lose its ability to put out an adequate level of thyroid hormone, then the anterior pituitary starts to crank up the levels of TSH that it sends out, hoping to get the thyroid gland to produce more thyroid hormone. So, usually, as one becomes hypothyroid TSH goes up.
In terms of effects on appetite and body composition the main effects are indirect. As your body uses less energy (low thyroid) more of what you eat gets stored as fat. As your body uses more energy (high thyroid) you tend to lose weight.
This has led, over the years, to a recurrent idea that the solution to being overweight is to crank up the thyroid.
The problems with this approach are –
- Overshooting your body’s natural thyroid level results in other negative effects which outweigh any effects on weight – early osteoporosis, cardiac problems.
- High thyroid tends to have only a modest effect on weight loss
Sex Hormone Systems
These systems have more profound effects on body composition than we have really been aware of up until the last few years. Testosterone (in both men and women) regulates muscle mass. And estrogen (in both men and women) regulates fat stores.
Testosterone increases muscle mass and strength. And low testosterone is associated with loss of strength and may be a major source of disability in older people.
Estrogen turns out to have an important role in fat regulation in both men and women. As estrogen levels fall (after menopause for women) fat stores tend to increase. In men the blood level of estrogen is determined by how much testosterone there is – testosterone gets converted to estrogen – so as testosterone levels fall, estrogen levels go down, and that, in turn, leads to more fat deposition. 
Before the recent research on the benefits of higher levels of estrogen, in men and women, in terms of reduced level of body fat, the fact that testosterone is converted to estrogen in the body (particularly, as it happens, in fat cells) had led to prescribing medicines to block that conversion. Medicines which may, inadvertently, have contributed to increased body fat.
Whereas estrogen supplementation in men is probably not a good idea, this may lead to another reason to use testosterone supplements in older men.
The Insulin System
The insulin – glucagon system serves to regulate blood sugar. Blood sugar is critically important to a number of organs that rely almost exclusively on blood sugar as a source of energy. Of these organs, the brain is probably the most important one. Low blood glucose rapidly leads to shutting down the brain, and ultimately to seizures and death. 
Again, maintaining high enough levels of blood sugar had always been the most important challenge, until we changed our diet and lifestyle and high blood sugar became an epidemic.
Nowadays the main problem is “insulin resistance.”
Some people, in the presence of a diet rich with simple carbohydrates and a lifestyle with little exercise, become increasingly resistant to the effects of insulin. There appears to be a strong genetic basis to this tendency – some native american populations have incredibly high rates of diabetes in this century.
Insulin basically stimulates the body to use blood sugar. Insulin resistant cells can’t use the blood sugar, and because they can’t use blood sugar, the body develops abnormally high levels of blood sugar that are associated with damage to various organ  systems.
systems.
The metabolic syndrome is the combination of insulin resistance, elevated cholesterol (along with other lipids) and hypertension. Although the exact way that this syndrome develops are not entirely clear, it does appear that early intervention with lifestyle changes, and, often, medication like metformin that enhance insulin sensitivity may help to prevent some of the adverse consequences of this condition.
Paying attention to the literature in this evolving area is probably a good idea.
